Citation: Welch B, “Critical Considerations in Choosing High Viscosity/High Volume Drug Delivery Devices”. ONdrugDelivery Magazine, Issue 83 (Feb 2018), pp 50-53.
There are some device design considerations that are common across the spectrum of biologics development. Bill Welch discusses these considerations, highlighting the advantage conferred by accounting for them early in the product lifecycle.
With the ongoing increase in biologics development, early involvement between drug manufacturers, device designers and device manufacturers is critical to the development of an effective and efficient drug/device lifecycle strategy. Many biologics are highly concentrated, so a prescribed dose may be very viscous, or require large volumes of the medication to be injected slowly over time. This can make it difficult to deliver a consistent dose, potentially impacting patient adherence to a given therapy, and so it naturally follows that device development considerations should begin as early as possible.
“Upon first consideration, the simplest solution would be to increase the needle diameter, thereby reducing plunger force to accommodate a more viscous formulation. However, a larger needle would increase pain at the site of injection, decreasing patient acceptance and adherence…”
These particularities of biologics have led to a rise in the popularity of wearable self-injection systems. Instead of scheduling a doctor’s appointment for certain treatments, a wearable device allows patients to self-administer large volume injectable medications. Some estimates predict that, by 2020, biologics will make up more than half of the world’s top 100 selling drugs. To keep pace, device designers must needs overcome the myriad challenges associated with delivering these drugs.
Chief amongst the issues associated with biologics are those of high viscosity and high volume. For proteins, issues of viscosity, solubility and protein aggregation become major obstacles, especially with the smaller-gauge needles that patients prefer. Biologics cannot be taken orally, so the question of how to deliver them via an injection, in a fashion satisfactory to the end-user, cannot be circumvented. Whilst these challenges are not unique to biologics, these drugs demand special attention from device developers.
DEVICE DESIGN CONSIDERATIONS
From a delivery device perspective, higher viscosity drugs require more force to push fluid through the narrow orifices used in delivery, for example a cannula. This force, or “syringeability” as it often called, is dependent upon many more factors than formulation viscosity alone, including desired flow rate, needle length and needle diameter. Any small change in the needle diameter will result in a large change in the plunger force.
Upon first consideration, the simplest solution would be to increase the needle diameter, thereby reducing plunger force to accommodate a more viscous formulation. However, a larger needle would increase pain at the site of injection, decreasing patient acceptance and adherence. But then again, maintaining a smaller needle will lead to higher than “normal” plunger force, leading to user fatigue and poor user experience. So, the conundrum for device designers is obvious, how best to balance these two opposed design problems and create the most positive user experience possible?
AUTOINJECTORS
One solution is the use of an assisted delivery device, a common example being autoinjectors such as those used for epinephrine delivery. These can be fitted with power sources that drive the plunger at forces higher than could be provided comfortably by the user. This approach enables device designers to maintain a smaller gauge needle and place the burden on the power source to provide the high force needed for delivery. However, this approach comes with its own set of concerns and considerations (Figure 1). These include:

Figure 1: It is imperative to consider all aspects of a device early in the design process, and how each factor will impact usability and patient adherence.
Size
A power source capable of providing the force required to push large molecules through a small needle is often physically large. This goes contrary to market trends, which suggest that users prefer smaller devices.
Material
New high-strength materials can be used to help alleviate the aforementioned size issue by deploying smaller wall sections and structural features in devices and container closures, thereby miniaturising them. New material technologies can also be used to derive power sources, usually springs, that are smaller and yet provide the same forces.
Safety
Stored energy devices, such as springs under compression, require robust safety features to prevent injury, device failures and accidental actuation. Where devices are delivering viscous drugs, this is crucially important. An accidental drop, material fatigue, failure of the glass container closure or excessive vibrations can lead to catastrophes that could injure users or prevent lifesaving drugs from being administered.
The autoinjector approach focuses on maintaining a smaller needle diameter by accepting a higher plunger force. This approach centres on different ways of executing a high force power source. Another approach could be reducing plunger force, whilst still maintaining a smaller gauge needle, by simply lowering any of the variables in the numerator of the Hagen-Poiseuille equation, assuming pressure at the needle is constant:

“The conundrum for device designers is obvious, how best to balance these two opposed design problems and create the most positive user experience possible?”
Where:
- F is the plunger force
- L is the length of the needle
- μ is the viscosity
- Q is the flow rate
- A is the area of the plunger
- D is the internal diameter of the needle.
One possible change would be to reduce the diameter of the plunger and thus the plunger area. However, this has size implications, as the syringe or device would need to become longer to accommodate the same drug volume, which raises further problems. Alternatively, the flow rate could be reduced, lowering the force but increasing delivery time. Likewise, decreasing viscosity can be achieved through dilution but the increased volume also increases delivery time. Therefore, these solutions require a different delivery approach that cannot be achieved through direct injection methods.
WEARABLES
IV delivery is the extreme case. IV solutions have a much reduced viscosity over syringe based formulations, as well as a significantly reduced flow rate. However, this method greatly prolongs the delivery time. Whilst patients may accept this form of delivery for otherwise unavailable therapies, quicker and more convenient delivery methods are always preferred and are vastly more suitable for non-clinical settings. In response to these limitations, body-worn infusion pump devices may be an alternative worth investigation and investment.
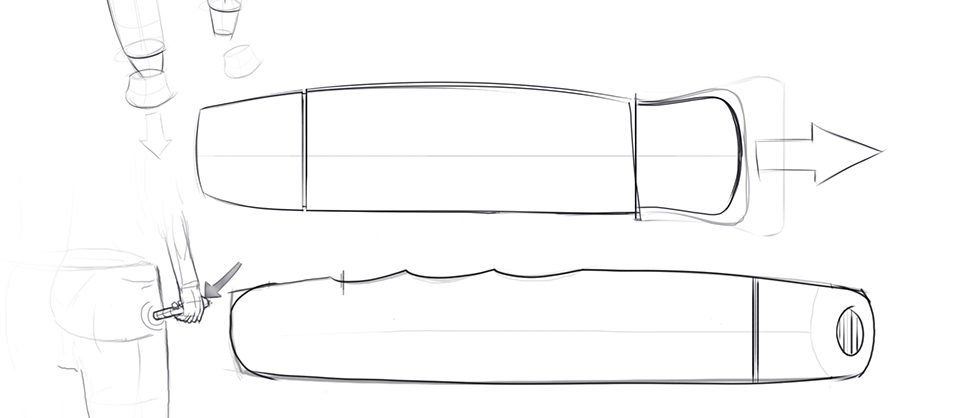
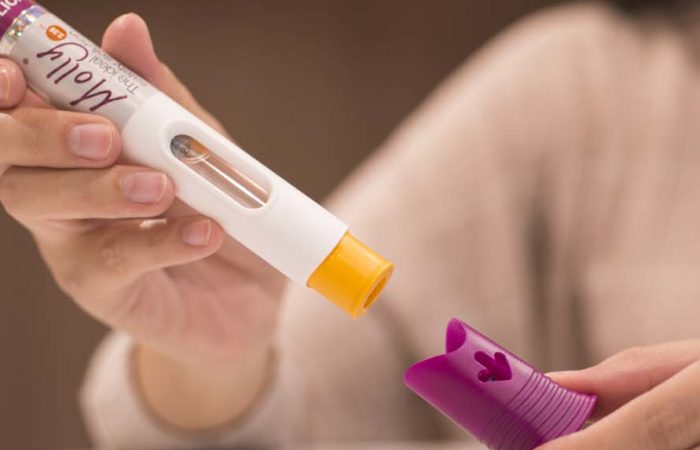
These are already common in diabetes treatment, in which users wear an insulin pump connected to their body via a cannula. However, for delivering high volume drugs, a different perspective is required: the device needs to be treated as a prolonged injection device rather than a continual-use pump (Figure 2). Ergo, such wearable injectors carry their own new set of challenges:

Figure 2: An example wearable injection device.
Size
The size challenge in body worn devices lies in the necessity to slow down the delivery speed. While the delivered force required to push the drug through a needle may be smaller, it needs to take place over a period of several minutes to a few hours. Any additional components that may be required to modulate the delivery rate will require more space, causing an undesirable creeping increase device size.
“Unlike prefilled syringes or autoinjectors devices, where the user maintains constant interaction throughout the injection, users of body worn devices cannot be expected to remain vigilance over the course of the procedure, which may take several minutes or even hours…”
User Interface
Unlike prefilled syringes or autoinjectors, where the user maintains constant interaction throughout the injection, users of body worn devices cannot be expected to remain vigilance over the course of the procedure, which may take several minutes or even hours. Therefore, the ability of the device to provide error alerts, indicate progress and confirm delivery becomes critical, freeing the user to perform other activities whilst the wearable injector does its work.
Body Fixation Method

Figure 3: Where a wearable device is to be worn is a crucial factor to consider, alongside the components of the device itself.
The first challenge with wearable devices is where they should be placed on the body (Figure 3). There are numerous questions that must be considered before a conclusion can be drawn:
- How sensitive is the tissue?
- Can an adhesive be used on this part of the body?
- Is the adhesive aggressive enough to hold the device in place over the required time period?
- Will it cause allergic reactions?
- Could or should a band of some description be used instead of an adhesive?
- Will the device need to survive wet conditions or withstand physical activity?
- How will the patient feel about wearing a device, is it obvious or obnoxious?
- Will the skin surface need to be shaved before application?
- Does the patient feel “tethered” by their device?
Another consideration is looking at alternate injection platforms departing completely from the conventional needle based designs. Microneedles and needle-free technologies are potential alternatives that could be explored for delivering high viscosity and/or high volume drugs.
Human Factors Considerations
As evidenced by the US FDA’s increased attention to human factors considerations in their appraisal of drug delivery devices, a thorough investigation of a user’s interaction is as important as the actual performance of the device. A device that is difficult for a patient to understand or use intuitively, even if it performs sublimely under perfect conditions, can detract from compliance. As such, device developers will often conduct design and manufacturing process failure mode and effects analyses (FMEAs) early in the product lifecycle. Discovering a significant potential use error, once the development or manufacturing phase has begun, can be costly.
“Connected devices are becoming more prevalent in the healthcare sector, as tech companies turn their attention to drug delivery devices and device designers take more note of the benefits connectivity has brought to other industries…”
CONSIDERING CONNECTIVITY
Connected devices are becoming more prevalent in the healthcare sector, as tech companies turn their attention to drug delivery devices and device designers take more note of the benefits connectivity has brought to other industries. These benefits include monitoring patient compliance, tracking user activity and location to customise patient care, and managing refills. But these benefits need to be weighed against the implications of their deployment.
- What are the regulatory implications of including these technologies?
- Can third party apps be permitted and, if so, will necessary software updates be managed?
- How will the distribution of apps be managed for drug delivery devices?
- How will the user data, and the entities that hold and manage it, be regulated?
- What are the infrastructure implications?
- Who will manage user data?
- Will user data need to be anonymised?
- Which connectivity technologies should be used?
- How should device recycling or disposal be managed, is conventional sharps disposal compatible with electronic devices?
- Is hacking a threat and, if so, what is the best way to protect against it?
CONCLUSION
Manufacturers of devices will continue to repeat the mantra of “early engagement” with device designers and developers. This stems from the simple premise that it is easier, cheaper and quicker to make the inevitable change to a design at the beginning of the development cycle than it is toward the end. Manufacturing issues discovered after a design has been locked can cause severe delays or even derail the entire programme. This thought process applies to the drug developer and device designers alike, as earlier considerations regarding device strategy can avoid crippling challenges down the road.
Of course, it is worth restating, here at the conclusion, that the most critical and central consideration for device designers must always be the wellbeing of the patient.