To Issue 158
Citation: Needham M, “The Evolution of Pulmonary & Nasal Drug Delivery”. ONdrugDelivery, Issue 158 (Apr 2024), pp 8–10.
Mike Needham takes a look at the history of, and progress in, inhalation technology and discusses what might lie ahead.
Physicians have treated illnesses with inhaled remedies for thousands of years. The pressurised metered dose inhalers (pMDIs) used today differ dramatically from the pipes, reeds and pots used centuries ago – but the benefits of inhalation devices have stood the test of time. As the inventor of the original pMDI, Kindeva Drug Delivery draws on this legacy to develop the pulmonary and nasal innovations of the future.
PULMONARY & NASAL DELIVERY: ANCIENT TO MODERN TIMES
The first known reference to therapeutic aerosol delivery dates to about 1554 BC. It describes Egyptians who were struggling to breathe fumes from heated plants. The delivery mechanism was a reed placed in a jar with a hole in the top. Plants were placed under the jar on hot rocks, then people inhaled the medicinal vapours through the reed.
Incense burners, pipes and funnels were popular mechanisms for inhaling herbs for medicinal and recreational use between about 1100 BC and the mid-1700s. These devices delivered a variety of inhaled treatments for asthma, cough and other lung and nasal problems.
“The pMDI’s debut advanced the landscape of therapeutic aerosol delivery.”
The rise of manufacturing during the Industrial Revolution led to the first mass-produced therapeutic aerosols. Nebulisers and dry powder inhalers (DPIs) were introduced during this time. English physician John Mudge coined the term “inhaler” in 1778. The Mudge inhaler, which looked like a teapot with a long nozzle, was the first known commercialised inhaler device.
Dr Auphon Euget-Les Bain developed the first atomiser in 1859 in France, but it involved directing a jet of mineral spring water against a spa wall. Nine years later, Jean Sales-Girons developed a portable version called the pulverisateur. The first plastic nebuliser arrived in the 1950s, shortly followed by other devices that used compressed gas.1
KINDEVA DELIVERS THE FIRST METERED DOSE INHALER
The early atomisers and nebulisers informed innovation through the 19th and 20th centuries. However, the pMDI’s debut advanced the landscape of therapeutic aerosol delivery. Kindeva (then called Riker Laboratories) introduced the first pMDI in 1956. Over the following decades, the industry experienced unprecedented growth, improving quality of life for hundreds of millions of individuals.
A second wave of innovation occurred in 1987 with the signing of the Montreal Protocol on Substances That Deplete the Ozone Layer. That landmark agreement regulates the production and consumption of nearly 100 ozone-depleting substances. Inhaler technology has since diversified with enhanced delivery efficiency, updated DPIs and more advanced nebulisers. Kindeva played a significant role in this innovation with the launch of Maxair in 1986 and the Maxair Autoinhaler in 1992.
THE ARRIVAL OF GREEN PROPELLANTS
The inhalation technology space went through another round of innovation involving the elimination of chlorofluorocarbons (CFCs). Kindeva broke new ground in this space by getting the first US FDA-approved pMDI to use a hydrofluoroalkane (HFA) propellant on the US market in 1996. Since the last of the CFC propellants were phased out in the US around 2011, the industry has saved huge amounts of chlorine from entering the atmosphere and thereby greatly reduced the impact of inhalers on both ozone depletion and atmospheric warming. However, the journey continues as today’s pMDIs still use propellants with significant global warming potential (GWP), which can now be improved upon.
“Unlike some CDMOs that have moved away from pMDI development, Kindeva believes their ongoing optimisation is essential.”
While the current HFA propellants have a much lower greenhouse impact than the original CFC propellants, standards change. The impact of these gases (over 1,000x that of CO2) is now unacceptable as the world works to reduce the human impact on the climate. The time has come for another change to the propellants used in pMDIs, and the industry is moving toward incorporating greener propellants into current and future products to create a sustainable future. Once again, Kindeva is leading the charge to bring these greener propellants to market.
GREENER COMBINATION PRODUCT MANUFACTURING
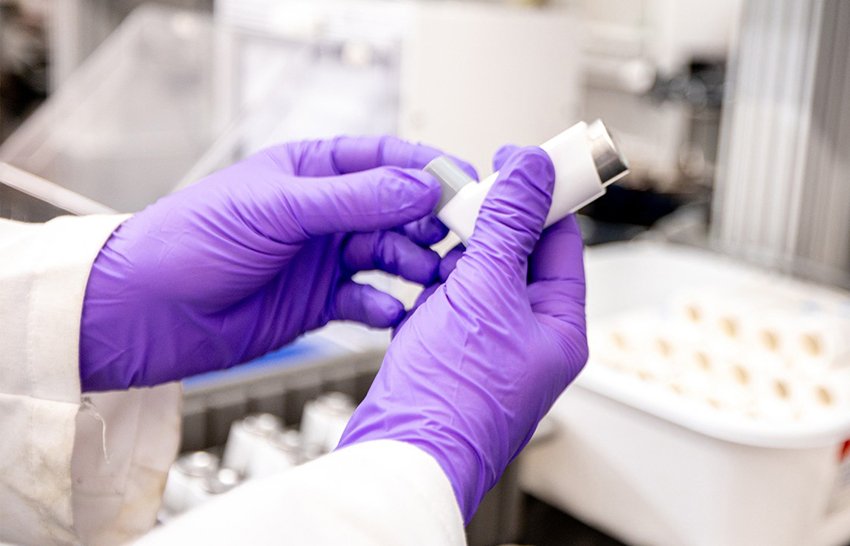
The move to the new generation of propellants requires significant investment in R&D capacity to accommodate not only the increased demand for these sustainable and reformulated products, but also for whatever developments come next. Unlike some CDMOs that have moved away from pMDI development, Kindeva believes their ongoing optimisation is essential to manufacturing more tomorrows for patients around the world (Figure 1).

Figure 1: Manufacturing components for an inhalation device.
With the introduction of greener HFA-152a and HFO-1234ze propellants, pharma companies have attractive alternatives, as these propellants have GWPs that are 90% and 99.9% lower, respectively, than P134a – the greenest pMDI propellant currently in use.2 To accommodate emerging demand, Kindeva has installed a pilot-scale manufacturing line capable of filling inhalers with HFA-152a or HFO-1234ze propellants. Clinical supply is already available, and the company is currently installing a commercial green propellant line set to begin production in 2025, making Kindeva one of the first CDMOs to do so.
By helping sponsors bring greener products to market as early as possible without compromising safety and quality, Kindeva is helping to ease the transition to new HFA propellants without impacting the current availability of much-needed treatments. And, once these greener products reach pharmacy shelves, the odds are strong that physicians will prescribe the more sustainable option, driving market share.
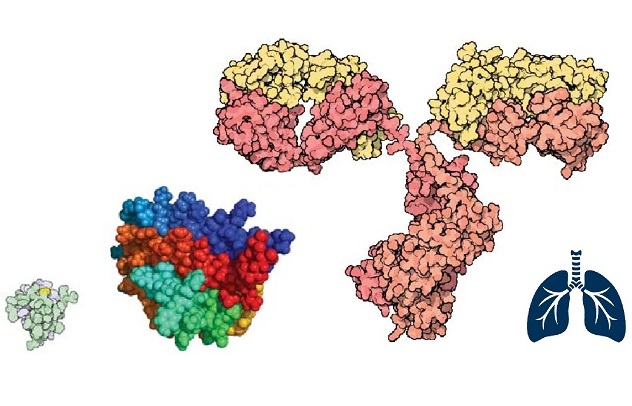
THE NEXT INHALATION FRONTIER: BIOLOGICS
A relatively new type of product is coming to inhalation that early adopters centuries ago could not have imagined: biologics. Small-molecule products will remain a staple for years to come, but large-molecule therapies are expected to become more prevalent and likely to come to dominate the market. This is as true for inhaled therapies as it is other routes of administration, the approach for pMDIs,DPIs, nasal sprays and others will remain therapy specific, as it is today – and Kindeva expects to continue to be at the forefront of this innovative technology.
To develop and manufacture these products, changes to how materials are handled and analysed will be essential. Evaluations of stability and the resulting drug delivery adaptations will drive this next product evolution. Kindeva is up to the challenge. With a long legacy of firsts in the pMDI space, the company is ready to scale and adapt to the next wave of inhalation innovation.
To find out more about green propellants, inhaled biologics or other pulmonary and nasal drug delivery platforms, visit: www.kindevadd.com/pulmonary-nasal-delivery.
REFERENCES
- Stein SW, Thiel CG, “The History of Therapeutic Aerosols: A Chronological Review”. J Aerosol Med Pulm Drug Del, 2017, Vol 30(1), pp 20–41.
- Fidler L, Green S, Wintemute K, “Pressurized metered-dose inhalers and their impact on climate change”. CMAJ, 2022, Vol 194(2).